Overview & Definition
Promising new chemical entities are screened based on their receptor binding ability, effects produced on the enzyme activity, cytotoxicity or other adverse outcomes screened in vitro, and other pharmacological factors. All potential drugs that have surpassed the initial screening are subjected to in vivo animal testing at the pre-clinical stage. In later phases, a single optimized lead is selected and characterized for the IND (Investigational New Drug) or BLA (Biologic License Application) application to request trials in human volunteers. In most cases, the approved investigational drug is first subjected to evaluation strictly in healthy volunteers at the initial clinical evaluation stage.
Before testing these drugs on human volunteers, the pharmaceutical company must file an IND or BLA application before the US FDA and/or other concerned drug regulating authorities. This application should be inclusive of all the pharmacological and toxicological data retrieved during the entire course of the drug evaluation in the animal population. Regulators require extensive toxicology evaluations in at least two preclinical species, one rodent and one non-rodent, prior to IND or BLA filing and clinical evaluation. Following IND or BLA approval, the new drug undergoes rigorous clinical trials with the goal of filing an NDA (New Drug Application) with the US FDA and other regulatory authorities for market approval.
The design of animal studies should be executed in such a way that the clinician can select a safe starting dose to be administered to humans. For most novel therapies, the initial clinical dose is low, often sub-efficacious, to ensure there are no unexpected adverse events. As the clinical trial results are gathered, doses are meticulously monitored and conservatively escalated to maintain safety, establish definitive clinical therapeutic doses, and confirm efficacy and tolerability. This helps the researcher evaluate the toxicity targets and establish a distinction between a therapeutic and toxic dose, known as the therapeutic index, the ratio between toxicity and efficacy. Compounds with narrow therapeutic indices must be more carefully monitored for side effects and adverse events. Pharmacokinetic and pharmacodynamic parameter evaluations are performed throughout this process to understand the novel drug’s disposition and activity in the body. As these are required by the global regulators, and are the preliminary stages of a drug development process, they usually turn out to be resource-intensive. In other words, you can say that a pharmaceutical or biotechnology company interested in developing a new product should be prepared to make significant investments in the synthesis and testing of the product of interest, use of animal, laboratory, and analytical processing, and, most importantly, time.
Objectives for introducing guidelines for IND Enabling Toxicology Studies
- Any pharmaceutical product being developed should undergo a thorough evaluation of safety in both animals and humans.
- The FDA guidance recommends international standards for harmonized non-clinical studies and their promotion. These are pre-requisites for setting a foundation for the human trials to be conducted for the same defined scope and duration.
- Non-clinical characterization of any pharmaceutical product is mandatory for marketing approval.
What are toxicological studies?
Toxicology studies are critical to the pharmaceutical product development and approval process. Pre- or non-clinical toxicology testing is required in a minimum of two species (one rodent and one non-rodent) by the US FDA and other regulatory agencies. These studies are conducted under 21 Code Federal Regulation Part 58, Good Laboratory Practice for Nonclinical Laboratory Studies to ensure appropriate handling of test subjects and reliability of scientific results. Most novel chemical entities will demonstrate adverse events or toxicity when dosed at a high enough level. Preclinical toxicity and toxicokinetics studies help determine if the drug is reasonably safe for initial tests in humans and define the margins between therapy and overdose. Adverse events noted during preclinical evaluations help clinicians monitor test subjects for potential undesired or unsafe effects. Knowledge of target organ effects related to toxicity help clinicians closely monitor patients and limit or withdraw therapy to prevent risk to human life or well-being. Thus, toxicology and toxicokinetics (TK) studies aid in the understanding of both the severity and reversibility of the toxic effects produced by a drug on a human body in general and on target organs in specific. TK studies evaluate wide dose ranges and how they relate to systemic exposure in the body. In other words, you can say that TK studies help researchers to determine exposure linearity with respect to dose, metabolic saturation, accumulation of compound and steady-state exposures, and related potential adverse events and the systemic exposures where they occur.
How does an exploratory IND study help a pharmaceutical company?
Exploratory IND studies, also referred to as clinical screening studies or microdose studies, are defined by the US FDA as clinical trials conducted early in Phase 1, involving very limited human exposure, and having no therapeutic or diagnostic intent. These studies allow organizations to assess feasibility for further development of the drug or biological product prior to dose escalation, safety, and tolerance studies normally tested in early clinical programs. Since these studies involve administering either subpharmacologic doses of a product, or doses expected to produce a pharmacologic, but not a toxic, effect, the potential risk to human subjects is less than for a traditional Phase 1 study that, for example, seeks to establish a maximum tolerated dose. Because exploratory IND studies present fewer potential risks than do traditional phase 1 studies that look for dose-limiting toxicities, such limited exploratory IND investigations in humans can be initiated with less, or different, preclinical support than is required for traditional IND studies. While the doses are sub-efficacious, these studies still provide valuable information:
- Evaluate whether a mode of action executed by the drug under analysis in the in vivo animal testing produces the same results when administered in the same dose and through the same route of administration in humans via biomarker analysis.
- Provide insights about the clinical pharmacokinetic characterization of a drug product.
- Out of the entire candidature list, shortlist the most promising candidate for the next stage of clinical evaluation. This is done in accordance with the drug’s PK/PD characterization.
- Explore biodistribution of the pharmaceutical product under analysis with imaging techniques.
Pre-clinical In-Vivo toxicology –
Pharmacological GLP toxicology studies are performed to understand the onset, degree of severity, and time length up to which a particular dose of a drug demonstrates any toxic effects. The dosing regimens for such studies usually range from acute studies where you have single-dose administration to chronic studies with multiple-dose administrations (route and time of administration being the same in both the cases). A particular drug under investigation can be administered through several routes such as oral, intraperitoneal, intravenous, topical, or intramuscular. Except in rare cases, the route of administration used in toxicology studies typically matches the intended dose route for use in the clinic. For pre-clinical studies, available animal models include mice, rats, guinea pigs, rabbits, and rarely hamsters for rodents, and canines, minipigs, and non-human primates for non-rodents. The choice of the animal models is made in accordance with the biological target for which the drug is being developed. While rats and dogs are most commonly used for toxicology studies, other species may be selected depending on the therapeutic area. For example, monkeys are often chosen instead of dogs for treatments of metabolic diseases since non-human primates more closely mimic humans for these disease targets. A full complement of the toxicology/TK study includes clinical chemistry, pathology, histopathology, measures of cardiac and pulmonary safety, ophthalmology, urinalysis, hematology, bioanalysis, toxicokinetic analysis, and statistical analysis.
Test categories for the In-Vivo Toxicology testing –
The test categories defined for the In-vivo Toxicological testing are as follows –
- Dose-Range finding
- Acute systemic repeat-dose toxicity for 3 to 7 days
- Subacute repeat-dose toxicity for 14 to 30 days
- Subchronic repeat-dose toxicity for longer than 30 days
- IND Enabling Studies
- Dose Escalation Studies
Services available with NorthEast BioLab for GLP toxicology studies of FDA
Dose-range finding –
Dose Range Finding at NorthEast BioLab provides quick and accurate toxicological and toxicokinetic analysis report of all the new potential drug candidates. Here, a drug is subjected to different study doses and is administered accordingly so that generalized evaluations of the maximum tolerated or maximum feasible dose and the therapeutic index can be made.
Single and Repeat-Dose Toxicity Study –
A single vs multiple dose toxicology study with toxicokinetic (TK) analysis is usually carried out in two different mammalian species before its administration in the human population. Single administration dose-range finding studies are often performed prior to multiple dose toxicology studies to establish the dose range for toxicology and TK analysis. The duration of chronic dosing for performing the repeat dose toxicity study depends on 3 significant factors of your proposed clinical trials – duration, scale, and a therapeutic indication of your pharmaceutical product under analysis. It is again performed in two different mammalian species, out of which one has to be non-rodent.
Acute, Sub-chronic, and Chronic studies –
Acute dose toxicity defines all the adverse health effects arising out of single-dose exposures and establishes the maximum tolerable dose level for single administrations.
Sub-chronic dose toxicity defines all the adverse health effects arising out of repeated-dose exposures administered at lower levels for a more extended period.
Chronic drug toxicity correspond to adverse drug effects arising out from the long-term exposure period to a specific toxicant or a stressor. Usually, it is considered with the direct evaluation of a direct lethality. Yet, it also comments on specific sublethal points such as behavioral changes, decreased growth, and reduced reproduction.
Determination of Local tolerance –
Local tolerance studies are used to evaluate any potential adverse events at the drug administration site, and are most often performed with parenteral administrations to determine whether there is any irritation or other undesired effects at the injection site. To perform local tolerance studies in animal species under pre-clinical evaluation, the route of administration should be maintained the same as that to be employed in clinical administration.
Biodistribution and Bioavailability –
Biodistribution evaluation of a pharmaceutical drug candidate is a form of in-vitro drug distribution or localization study. These are generally performed in non-clinical species, and the results obtained from them are used in support of the early stages of biotherapeutic drug development.
The term bioavailability refers to that fraction of the pharmaceutical product administered as an unchanged drug that reaches the systemic circulation following an extravascular dose. When any pharmaceutical product is injected intravenously, it is considered 100% bioavailable since the drug is dosed directly into the central compartment, or systemic circulation.
Other services are inclusive of –
- Evaluation of ocular and skin irritation
- Median Lethal Dose (LD50)
- Maximum Tolerated Dose
- No Observable Effect Level or No Observable Adverse Effect Level
Drug administration options available at the NorthEast BioLab
We, at the NorthEast BioLab, believe in evaluating a pharmaceutical product through all specific routes of administration. Therefore, we have the following options for drug administration at our facility –
- Capsule/solid formulation
- Dermal
- Oral gavage
- Intranasal
- Intratracheal
- Dietary admixture
- Subcutaneous
- Intraperitoneal
- Intravenous bolus
- Intravenous infusion
- Intramuscular
Species options –
We have a wide array of animal species for the evaluation of a particular pharmaceutical product –
- Ferrets
- Mice
- Guinea pigs
- Rabbits
- Rats or Cotton rats
- Dogs
- Minipigs
- Non-human primates
How to design a pre-clinical study trial
Here is an outline of how a pre-clinical GLP toxicology studies (FDA regulated) design should look –
- The main study objective is to evaluate the toxicity of a novel molecular entity (NME) in the test species using the intended clinical route of delivery and dosing regimen.
- Assessment of safety or toxicity in a healthy animal population with doses ranging from minimum efficacious dose to maximum tolerated (or feasible) dose.
- Regulations require preclinical toxicology studies be conducted under 21 CFR part 58, GLP.
- Animal welfare compliance must be addressed and protocols approved prior to execution by an Institution Animal Care and Use Committee (IACUC).
- Test article should be clearly characterized and defined, with a viable certificate of analysis (COA).
- Dosing vehicles and compound preparation should be clearly defined and dosing excipients used should be approved for the test model species.
- Test model species should be justified.
- Experimental design should include all intended doses, dose levels, routes of administration, and frequency and duration of administrations.
- Clear definition of animal observations required, including detailed clinical observations, body weights, ophthalmic observations, food consumption, and dermal observations
- Hematology, clinical chemistry, coagulation assays, urinalysis, electrocardiograms, and any other relevant safety measures with clearly defined endpoints.
- Pathology and histopathology as needed to evaluate target organ toxicities.
- TK analysis typically following a single-dose collected on the first day of dosing and multiple-doses collected on the last day of dosing. Known metabolites of the NME should be evaluated as well if they demonstrate significant in vivo exposures or therapeutic or toxicologic activities.
Standard Toxicology End-points –
- Mortality, body weights, clinical observations, and appetite
- Clinical pathology is inclusive of hematology, serum chemistry, urinalysis, and coagulation factor.
- Pathological findings for both target & non-target tissues to determine scheduled & unscheduled deaths; comprehensive gross pathology, histopathology, and organ weights; pathologists blinded to treatment.
- Toxicokinetic parameters necessary to describe compound exposures, multiple dose accumulation or steady-state exposures, dose linearity, saturable metabolism, gender or population differences, formulation comparisons, etc. depending on the compound properties and study objectives.
What animal data do you need to define your GLP toxicology studies to FDA?
The US FDA clearly defines the pre-requisites of every IND application necessary for review prior to initiation of clinical trials. These guidelines are readily available on the website of the FDA. (ICH M3 (R2) (Non-clinical safety studies for the conduct of human clinical trials for pharmaceuticals) is referenced for small molecules; while ICH S6 (R1) (Preclinical safety evaluation of biotechnology-derived pharmaceuticals) is referenced for large molecules).
An overview of the ICH M3 guidelines for the small molecules –
ICH M3 includes instructions for performing non-clinical safety studies to execute the human clinical trials for a particular pharmaceutical product.
ICH M3 provides a detailed outline for all the animal studies required to open an Investigational New Drug, and its respective NDA filing.
ICH M3 does not inform you about how to interpret your animal studies results.
For opening an Investigational New Drug, you need –
- Pharmacology studies (efficacy and proof of principle use of animals)
- A general TK assay study for rodents of at least 14 study days.
- A non-general TK assay study for rodents of at least 14 days.
- Data on genotoxicity studies
- Data on safety pharmacological studies
- Data on ADME characterization
- Analytical TK assays
General toxicological studies should comprise of –
General routine drug dosing to animal subjects through the same route of administration to be employed in humans.
Selection of the relevant species
- Metabolism should be parallel to humans if the drug is intended for therapeutic benefits to the human population.
- The animal species should possess the same target site for which the drug is being developed for humans.
- Some species may possess a little too high sensitivity to particular drugs such as rats are sensitive to the NSAIDs. At the same time, the dogs are sensitive to glucocorticosteroids.
- The selection of the relevant animal species and the count for the same should be made in accordance with the amount of the drug available for pre-clinical in vivo GLP toxicology studies.
Selection of the dose levels –
Usually, the in vivo toxicology studies is initiated with 3 dosing groups and a control group.
Apart from performing a 14-day toxicity study, the researcher must evaluate the pharmaceutical product for its bioavailability by subjecting it to a single-dose IV study in addition to the intended clinical route of administration.
General toxicology studies are inclusive of daily cage-side recordings of body weight, food and water intake; plasma samples for PK analysis which is usually performed on your last dosing day; clinical pathology at the end of your pre-clinical study and before the start of your actual clinical trials; necropsy; and finally histopathology.
Genotoxicity testing includes two different GLP in vitro tests –
Mutagenicity – Evaluation of DNA damage by subjecting the drug to several bacterial strains.
Clastogenecity– Evaluation of chromosomal damage Safety pharmacology studies are inclusive of single-dose studies, and higher dose studies for evaluating the maximum tolerated dose.
ADME characterization –
ADME characterization is a very crucial aspect of the evaluation to determine the fate of a pharmaceutical product after it enters a biological system. Here, you evaluate a drug for its absorption, distribution, metabolism, and, finally, its excretion from the system.
The information essential to sum up the ADME characterization of a pharmaceutical drug product is collected throughout the entire study duration. This helps you to understand the underlying mechanism of ADME effects of your drug at the IND filing stage itself.
Analytical TK assays –
- TK assays must be fully validated according to the FDA bioanalytical guidance for industry for all GLP toxicology studies.
- They are crucial for the quantification of drug plasma levels.
- If your test article involves complex metabolism, the analytical assay procedure must include evaluation of significant concentration or active metabolites which must be evaluated individually for toxicology and TK.
- Analytical TK validations and assays are essential for demonstration of test compound and metabolite selectivity and specificity.
An overview of the ICH S6 for biologics –
- Data on the pre-clinical evaluation of the safety parameters of the biologically derived pharmaceutical products.
- General toxicology in monkeys and its changing requirements when performed on mice or rats.
- There is no special requirement of genotoxicity studies according to the ICH S6 guidelines.
- Like the ICH M3 guidelines, you need safety pharmacology data to be generated for biologics.
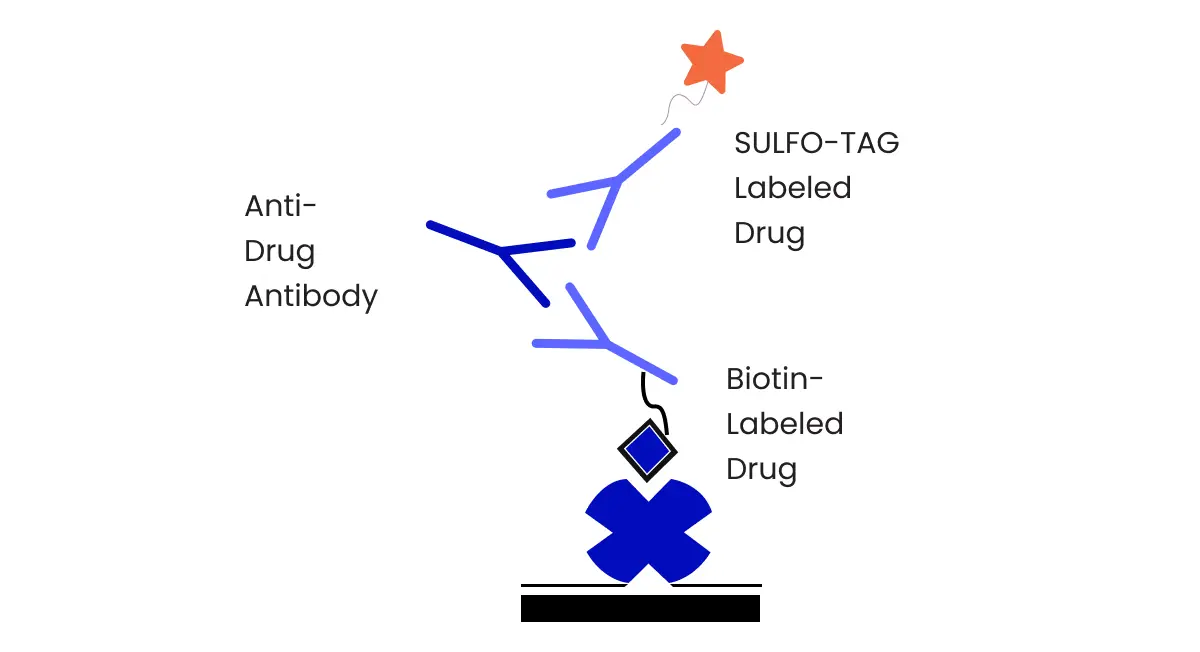
- Immunogenicity testing is required using monoclonal antibodies.
- ADME characterization of the biologic pharmaceutical drug product.
What sources of data can you use for supporting your IND’s pre-clinical or clinical evaluation?
Select reference materials to establish the pre-clinical or clinical characterization of your IND –
- GLP compliant toxicokinetic study design to be conducted by a certified and registered testing facility.
- Research through the published data available in peer-reviewed journals, which are similar or relevant to the pharmaceutical product under analysis.
- Cross-reference any similar products that have been previously submitted as IND’s.
- Detailed study reports generated from the clinical trials of the therapeutic bioequivalence conducted in the US or any other relevant countries.